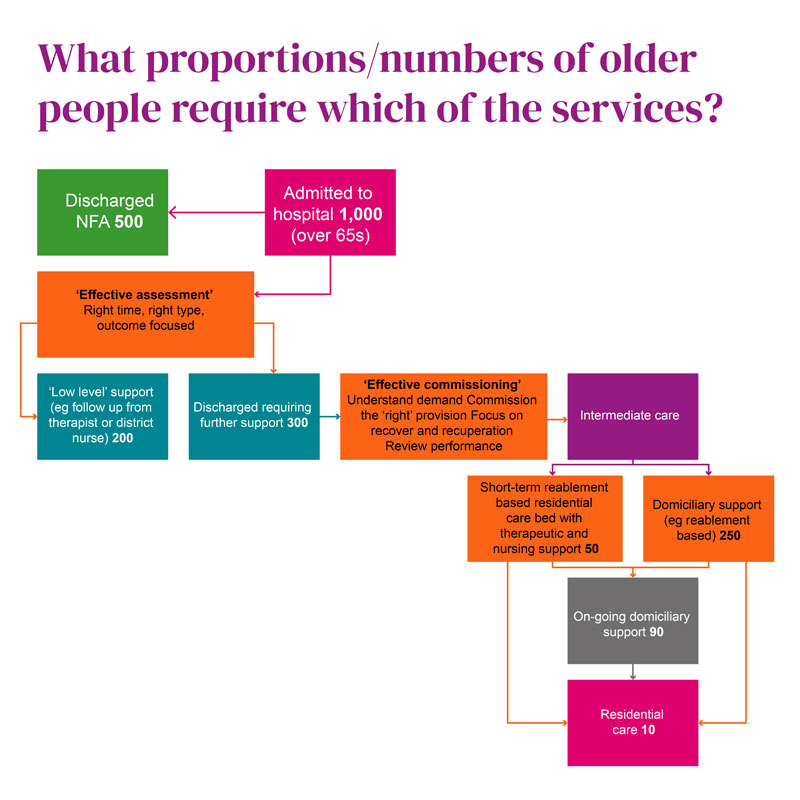
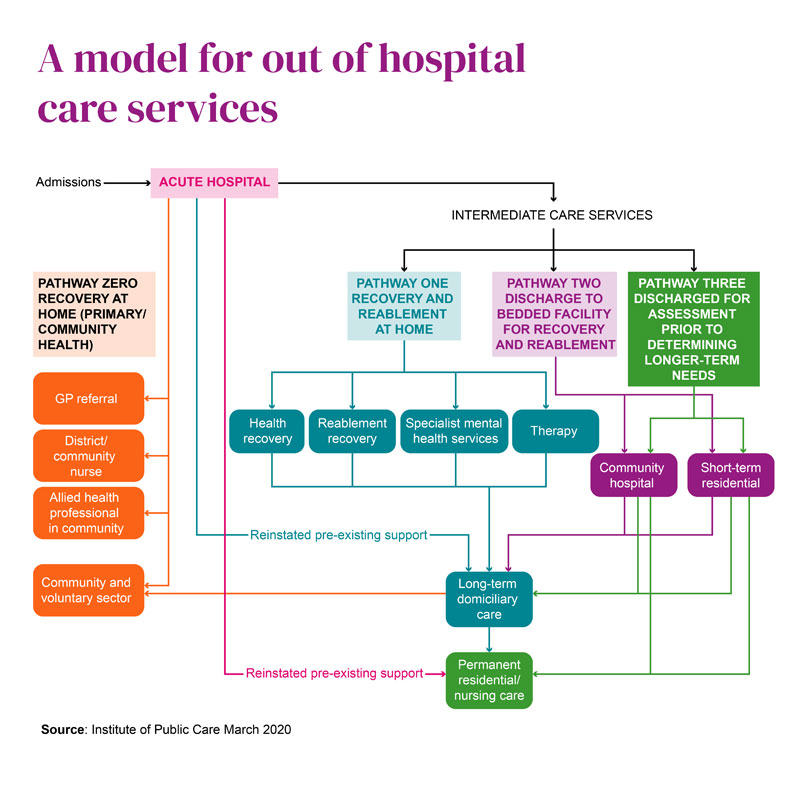
All the participants in this programme completed phase one. The key learning points that emerged from analysis of services available in each pathway included:
1. Different care pathways for people with similar needs
It was common for systems to have two separate care pathways for older people leaving hospital to go home (Pathway 1) - one commissioned or provided by the NHS (often referred to as a Home First service; the other commissioned or provided by the local authority (usually referred to as domiciliary care reablement-based service). There was often a lack of clarity as to which older person might be eligible for which set of services. In each place where this was the case it was agreed to either establish greater clarity on the role and purpose of each service, or to start work to integrate the services into a single model. In LLR there was a model where the NHS commissioned services took older people straight from hospital and then after 72 hours if they required more support, they were moved on to the Local Authority provided/commissioned services (reablement or domiciliary care). It also included a falls response service within two hours. This seemed to work particularly well in Leicester City. In North Tyneside discharges from hospital are co-ordinated through a single point of access, where care and health teams assess and provide support dependant on the person’s needs. There is also a first responder’s falls service that receives referrals direct from the ambulance service. The services are delivered through Care Point – a fully integrated health and social care intermediate care service. Stoke and North Staffordshire also offered an integrated response.
Ensure there are clear pathways across the NHS and the local authority for older people leaving hospital, where possible this should be through jointly commissioned or fully integrated services.
2. Commissioning of services from the voluntary sector
Most systems had commissioned a small volume of low-level post-hospital support from the voluntary and community sector it was recognised that this could be expanded to reduce some of the pressure on the community-based domiciliary services for both NHS and local authority. There is evidence in England (590 people's stories of leaving hospital during COVID-19) that both Age UK and the British Red Cross, as well as other smaller more locally based voluntary organisations, run excellent service (People's Stories of Leaving Hospital During COVID-19). Such evidence suggests many more people would benefit from some contact after their discharge to assist them to re-establish themselves at home, even if they don’t need domiciliary care and support, but they may benefit from a ‘take home and settle’ service and some practical reassurance. The programmes in Neath Port Talbot (Right Sizing Community Services to Support Discharge from Hospital) similarly show how the voluntary sector can offer a realistic alternative for many people to domiciliary care reablement and producing similar outcomes (Right sizing community services to support discharge from hospital). Commissioning services from the voluntary sector not only can improve outcomes for older people but also offers them a richer range of services that can help them not only with their recovery but also to regain important social links in their community.
There is tremendous scope to take pressure off Pathway 1 by developing flexible contracts with the local voluntary and community sector. The Five Pathway approach in Wales has a special pathway as a route out of hospital with support from the voluntary sector. There have been some discussions in England that there should be a ‘Pathway 0+’ that offers more than ‘no support required’ but less than ‘domiciliary support’ which might encourage wider use of this opportunity to gain speedier discharges and avoid deterioration for people with low support needs.
3. Commissioning of specialist mental health services for post-hospital care
In all seven places it was agreed that the lack of mental health service involvement in either the commissioning or the provision of services for older people with dementia was a significant gap in support. The lack of a community-based specialist set of domiciliary care services supported by assistive technology often meant that the only safe route for older people with dementia post hospital was to a care home (where specialist places for older people with dementia are also in short supply). Professor Bolton referred to the very positive impact that the services developed in Bridgend could demonstrate in the work undertaken by NHS Wales (Right sizing community services to support discharge from hospital). In Bridgend, the NHS and the local authority have jointly commissioned a dementia care service that specifically helps older people with a diagnosis of dementia or delirium to return home. This is seen as a vital part of their care pathway to support speedier discharges. Stoke referred to a couple of community support services run by a mental health trust (Marrow House and Harplands Ward 4) where assessments can take place for older people with a diagnosis of dementia, and a separate service for older people with complex needs which had a focus on reducing unplanned admissions to hospital for this group which included older people with dementia. It was recognised that many of the patients who are “stranded” in hospital have mental health needs alongside other complex conditions. There is an argument to be made that older people in the early stages of dementia are much more likely to “thrive” in their own homes where at least some things are familiar. This of course needs to be managed with the associated risks. This is an example of a cohort of people who may not benefit from a rehabilitation programme but do require specialist support to help them to live with dementia in their own homes. Some places have good assessment services that can identify quickly that an older person is experiencing a level of dementia – this is not an alternative to commissioning services that support those same older people in their own homes. In North Tyneside as part of the new integrated frailty pathway they have introduced mental health workers commissioned via Age UK. These workers link closely with other staff in the community including primary, community health services and Admiral Nurses.
Health and care systems must ensure that there is a range of appropriate specialist mental health services that can both support older people including those with dementia to return to their own homes (with the use of trained care professionals and assistive technology) as well as more specialist bedded facilities. Failure to address this guarantees a cohort of older people being prematurely and permanently admitted to long-term care directly from hospital.
4. The commissioning of bedded facilities
The role of bedded facilities to support discharge, where the focus is on recovery, was a topic of much interest from the participants. During the programme, the National Institute of Health Research (NIHR) published a study on inpatient care for older people in community hospitals (Measuring and optimising the efficiency of community hospital inpatient care for older people: the MoCHA mixed-methods study). This research shows the best evidence on how to set up and staff a multidisciplinary community hospital to be most cost effective and produce the best rehabilitation outcomes for older people. It was agreed by programme participants that community hospitals can play an important role in helping the timely discharge and then the recovery of older people who are assessed as requiring bedded facilities. There was broad agreement that the 70 per cent target set by Professor Bolton for older people to return home from a community hospital was realistic if the optimised staffing (including therapists) is in place. Obviously, this is different during the COVID-19 pandemic when some of these hospitals have played a specific role in managing post-COVID-19 care.
All participants realised that if older people were placed in care home beds for the purpose of Discharge to Assess but that no therapy or other recovery-based activity was offered to them, there was a very high chance that the person would remain in the care home for the rest of their lives. The data from several sites suggested that those placed in bedded facilities (short-term) where no support for recovery was available there was a 20 per cent chance, they would return home whilst for those placed in beds where recovery programmes were supported, then around 70 per cent were likely to return home. This emerged as one of the big challenges of the current arrangements in most places. The high death rate in care homes through the impact of COVID-19 had created spare capacity in the residential and nursing sector that created potential to facilitate rapid discharge for people needing a high level of support. However, simply buying these beds may have addressed the challenge of accelerating hospital flow but did not improve the outcomes for older people unless focused therapeutic or nursing support was put in to support active recovery and achieve the goal of returning home.
All bedded facilities should be commissioned for the purpose of recovery prior to an assessment of the older person’s needs. Most older people will do best in their own homes, but some will require the opportunity for recuperation and building personal resilience prior to return home. The bedded facility - whether in a care home or a community hospital - should have support for people to return home as its central objective. As a manager of community services (NHS) observed: “there are plenty of beds in the system available for use – they are in people’s own homes!”
5. Reinstating previously arranged domiciliary care
The role and nature of reinstated domiciliary care was also a point of discussion with the participants in some places. In some councils they keep open, for an agreed period, any package of care that was in place prior to a hospital admission so that it can be reinstated immediately on discharge. Obviously, this costs money but enables older people to be discharged quickly if they were already in receipt of care. The nature and frequency of support can be reviewed once they return home.
Local authorities should explore how cost-effective it might be for them to keep open packages of care for older people who are admitted to hospital to support rapid reinstatement and avoid delays.
6. The supply of domiciliary care
The supply of domiciliary care was presented as a major issue for both Leicestershire and Bristol City Council. Each requested a separate meeting, to focus on this issue, during the programme. The focus of the discussions had three aspects:
- To what extent was the shortage of supply related to the way in which the domiciliary care was procured and the relationship with the providers of care?
- Or to what extent was the over provision of care and the prescribing of too much care in some cases leading to a shortage?
- Or was there a shortage of supply and therefore different and new solutions had to be found?
Of course, all three dimensions are contributory factors to the problems experienced in many (but not all) places in England. The limited responsibility and flexibility given to care providers was clearly seen as one problem. There is a growing view that providers should be given more autonomy to work directly with their customers to flex packages of care according to their needs. Evidence from places that have piloted models that allow older people to direct their care providers (acting as trusted assessors) on a week-by-week basis without having to resort to a care management review were explored. Evidence from the effectiveness of different ways of supporting older people who pay for their own care (‘self-funders’) was also discussed. There was also evidence shared from the work in Somerset to develop community enterprises, in rural areas, that has had a positive impact in increasing the supply of people willing to offer care in both a paid and voluntary way.
There was common agreement that domiciliary care was a valued and precious resource. This means that it must be used carefully and flexibly.
The way in which domiciliary care is procured, the relationship with providers, the development of community alternatives, and how care is assessed and prescribed, all make a difference to the type and supply available in an area. Sometimes there is not a shortage of supply per se, but an over-use of the services that have been commissioned.
7. Reablement-based domiciliary care
All councils were either delivering or procuring reablement-based domiciliary care. Most understood the outcomes they were achieving although the very different results were not always understood. The important message is that reablement works best when it is part of a therapeutic plan to help the older person make some level of recovery related to their needs, as highlighted in research by the University of York and PSSRU, albeit now quite dated (Home care re-ablement services: Investigating the longer-term impacts). Those councils in this programme who had commissioned their reablement services from external providers often found that they had not included the importance of the therapist role in specifying these services and this then led to poorer outcomes (in relation to recovery) for service users. Councils were referred to the study of Coventry City Council’s excellent externally run reablement-based domiciliary care services included in a review of new developments in adult social care published by the Institute of Public Care.
All councils should ensure that their reablement-based domiciliary care services are following a therapist’s plan developed with the older person to help them to regain their confidence and physical capacity, and to support their post hospital recovery. Commissioners should know and understand the outcomes that each of these services achieves (whoever is the provider).
8. Frailty strategy
North Tyneside adopted a slightly different approach to the main programme. They were keen to participate in the programme but had already developed a local integrated frailty service which was in advanced stages of implementation during this programme. The strategy was over seen by an executive team drawn from both commissioning and operational leaders in the NHS and the local authority. The programme, therefore, looked to support the evolution of the work that was already being undertaken. In essence this was part of an admission avoidance programme using the same services to those used for patient discharges.
The new integrated frailty service was based on two pathways, one for urgent responses and one for planned responses. These are delivered through a single point of access where referrals are triaged and allocated to a range of services based on the individuals needs. One key issue that participants wished to explore was the best way they could measure the progress they were making. The measures that were developed and adopted by North Tyneside are included in the appendix to this report. Links were also established between the North Tyneside Integrated Frailty Project Group and personnel in the NHS Delivery Unit in Wales who were working on similar issues. Interestingly, when North Tyneside reviewed their existing provision to establish their frailty service, they recognised the need for community mental health services and created two posts to support the work in their new designed set of services.
Admission avoidance is equally important to a good discharge programme. However, the research evidence is less clear about the best ways to tackle this. Establishing some clear measures on the effectiveness of interventions that are in place is one way to help build this evidence base.
9. Multiple councils and multiple NHS Trusts
There are challenges where there is more than one council working in collaboration with a single CCG or single NHS provider. Each council has evolved their own way of doing things and developed their local services in a particular way which they think suits them. This does not make an authority good or bad, but it can make it very hard for the NHS to find the best way to collaborate (even less to integrate) with separate sets of services commissioned by different authorities each with a distinct set of purposes and varied outcomes. The evidence seems to indicate that out of hospital services are best delivered by a single integrated organisation, jointly commissioned for that purpose with control over a range of specific intermediate care services. The more varied the services, the harder it is to have clarity and agreement over care pathways. Perfectly competent councils working with good health services may not get this right unless they can agree on the best care pathways for local older people and commission services accordingly.
Some councils commented on the complexity of working with a range of different NHS Providers who were themselves not always operating in an integrated way – this was a common observation on the way in which mental health services failed to link with the rest of the system to support discharges. It was however notable in several places that the NHS providers of community services offered good leadership to the out of hospital care arrangements.
Where there is more than one local authority working with a single NHS set of organisations, work must be undertaken to ensure that there is agreement on the care pathway for local older people that reflects both the needs of the NHS and the local authority. In an ideal world local authorities should come together with NHS partners to build a single set of services with a clear pathway route out of hospital. The NHS needs to ensure that all its organisations work together to support this pathway.
10. Other issues
Recovery and recuperation
During the process of this programme, several conversations took place with people who were interested in the work being undertaken but not directly involved in the programme.
One of these discussions was with Dr Andrew Marshall, a community geriatrician working in Dorset. A particularly interesting feature of the discussion was exploring the difference between rehabilitation and recovery. Dr Marshall put forward a view that for many older people who may have multiple co-morbidities, the help they are likely to need at the point of discharge is support that assists them in adapting to their life at home living with their long-term conditions.
Many older people live at home (and prefer to do so) with some difficulty but find ways to cope. This is not the same as undergoing a rehabilitation programme where a person makes a full or partial recovery. Sometimes at the point of discharge an assessment may be made that the person is unlikely to benefit from further rehabilitation. The point being made is that this is not the same as a person not being able to adapt when they return home.
One of the important features of any out-of-hospital care system is to ensure that the services are supporting people and helping with that adaptation to the new challenges they face. The evidence from Dr Marshall suggests that this help is optimised when the older person returns home to familiar surroundings, furniture, and possessions, and it is hard to replicate this in other settings.
The goals for the recovery of older people leaving hospital should be realistic. Most older people want to return to their own home, but they may need to adapt to the way in which they need to manage at home. Helping people to achieve that is as important for some as helping with a full recovery which may be less realistic. However, a partial recovery that can enable an older person to return to their own home is a goal well worth achieving.
The operational model
There was much discussion in the programme about whether the best way to establish a coherent strategy and a sustainable intermediate care service was to ensure that there was a fully integrated governance structure with pooled resources. There was a desire in some of the systems to build and sustain a single operational model to achieve this. The models run by North Mersey and Somerset were cited as examples of good practice where this was happening.
However, it was clear that the existing approach to intermediate care in most places left the services disjointed and not serving the population well. There was common agreement that the principle of a recovery-based model was most likely to offer improved outcomes leading to speedier discharges and shorter lengths of stay. There was not full agreement on the governance that could oversee this. However, Stoke and North Staffordshire which had an integrated system did demonstrate that with some fine tuning of the services on offer that they were probably best prepared to deliver a comprehensive intermediate care system.
A fully integrated intermediate care service (or set of service) under the leadership of both main partners with a jointly appointed director to oversee and coordinate the services was the aspiration of many of these systems. This cannot be achieved overnight and having a shared vision and action plan on the developments that needed to take place to commission the services to achieve this was the best starting point.
Future funding arrangements
There was a high level of anxiety expressed in all places about the temporary nature of the current funding that was put in place by the Treasury to support out of hospital care. It is hoped and expected in all quarters that this level of funding will be continued and will be included in the mainstream funds for the new ICSs as laid out in the 2021 Government white paper: The pooled budgets that are supporting current work need to be secured for commissioners to be able to commit to the design and outcomes that the discharge arrangements require to be sustainable in the longer term.
When short-term funding is put in place to support any care system, the money can only be used for short-term fixes. It cannot be used to transform a service. Any staff taken on with the funding are likely to be offered short-term contracts, but mostly the money was used to fund short term packages of care. These may or may not have delivered improved outcomes for older people – the systems did not yet know this.
The Treasury is believed to be exploring how the D2A money was used and whether it saved any money elsewhere in the system. The only evidence that is available suggests that there have been shorter lengths of stay in acute hospitals because of discharges during the pandemic without any associated increases in unplanned readmissions of patients. There are potential savings from reduced use of bedded facilities both short and longer term, but we are not yet able to demonstrate these savings in these systems. There have always been savings made by those councils who commission effective domiciliary care reablement-based services which can reduce demands on longer term support packages.
It is hoped that the security of the services that are now being commissioned will be assured when the chancellor is able to secure the funding for the out of hospital care system. Failure to do so will risk undermining real progress that has been achieved and will jeopardise the opportunities for older people leaving hospital with the prospect of returning home and achieving some recovery and independence.